A study published in October of 2024 concluded that intraoperative ultrasound (iUS) is a useful tool in the identification of the posterior pituitary gland (PPG) during pituitary adenoma resection.*
Focusing on the use of endoscopic endonasal iUS to visualize the PPG during pituitary adenoma surgery, this study sought to identify the importance of the visualization during surgery in the avoidance of complications such as central diabetes insipidus (DI) and syndrome of inappropriate antidiuretic hormone secretion (SIADH) which can occur due to the manipulation of the PPG.
Read More
Topics:
Active Imaging,
Intraoperative Ultrasound,
Neurosurgery and Spine
When it comes to brain tumor surgery, precision is paramount to achieve optimal patient outcomes. Traditional imaging techniques, such as MRI scans, are invaluable for mapping out the tumor before the operation begins. However, the dynamic nature of the brain during surgery means these pre-operative images quickly become obsolete. This is where intraoperative ultrasound (iUS) steps in as a game-changer, providing reassurance when it matters most to both the surgeon and the patient.
Read More
Topics:
Active Imaging,
Intraoperative Ultrasound,
Neurosurgery and Spine
BK Medical continues to encourage and support surgeons incorporating intraoperative ultrasound (iUS) into their daily practice. We are committed to developing innovative ultrasound technology that provides high-resolution images in real time for soft tissue visualization. As iUS grows in popularity in cranial surgery, BK Medical is simultaneously working on improving our utilization in a variety of spinal procedures, ranging from tumor resections to minimally invasive fusion surgery.1
Read More
Topics:
Active Imaging,
Intraoperative Ultrasound,
Neurosurgery and Spine,
Minimally Invasive Surgery,
Endonasal
The Use of Intraoperative Ultrasound During a Robotic Caudal Pancreatectomy with Splenic Preservation
A neuroendocrine tumor (NET) is a rare type of tumor that can occur anywhere in the pancreas. Diagnosis and treatment of NETs depend on the type of tumor, its location, whether it produces excess hormones, how aggressive it is and whether it has spread to other parts of the pancreas.1
Dr. Marcos Belotto, Robotic Surgery Specialist at Celebration Florida Hospital, recently used a bk5000 ultrasound system during a pancreatic surgery case to help him locate a neuroendocrine tumor. Dr. Belotto has a PhD in Surgery from Hospital Sírio Libanês and a Masters of Surgery from Santa Casa de São Paulo.
Read More
Topics:
Robotic-Assisted Surgery,
Active Imaging,
Intraoperative Ultrasound,
bk5000,
General Surgery,
Pancreas
Unlike other markets or fields that are subject to fluctuations in supply and demand, the healthcare industry is driven by an unwavering commitment to providing the best possible care for patients. Urologists, in particular, recognize the profound significance of this mission. From performing targeted biopsies and developing minimally invasive treatment plans, urologists devote considerable effort to delivering optimal care.
Read More
Topics:
Urology,
bkActiv,
Active Imaging,
Intraoperative Ultrasound
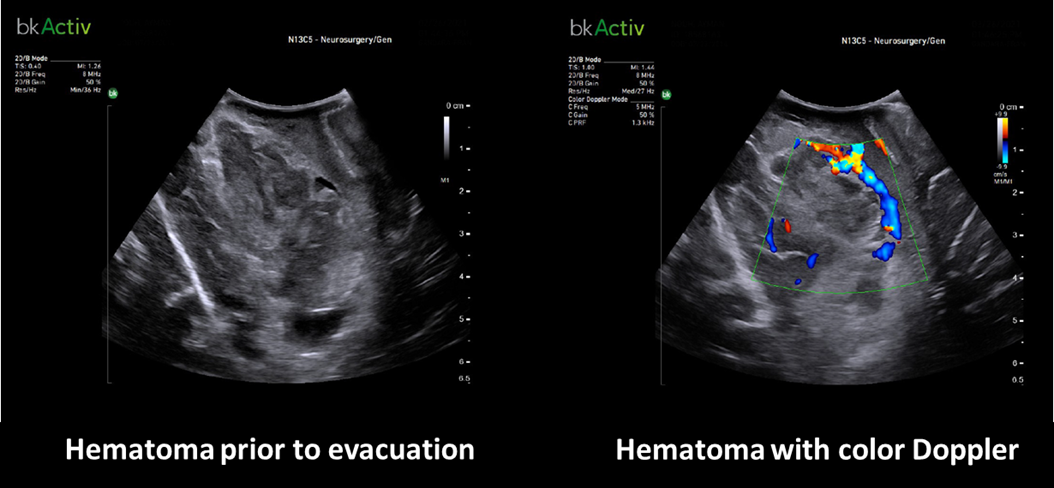
Dr. Fran Martinez Ricarte is the Coordinator of Neuro-Oncology and Radiosurgery at the Neurosurgery Service of Vall d’Hebrón University Hospital in Barcelona, Spain. He is a member of the Research Unit of Neurotraumatology and Neurosurgery at the Vall d’Hebron Institute of Research.
Read More
Topics:
Intraoperative Ultrasound,
Neurosurgery and Spine,
AVM Resection,
Hematoma Evacuation,
Craniotomy
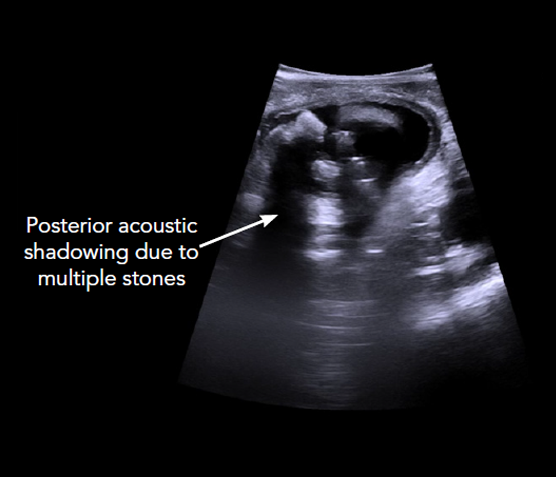
Mr. Somaiah Aroori, MB BS, MS (Surg), FRCS (Gen Surg) is a consultant hepatobiliary and renal transplant surgeon at Derriford Hospital and University Hospital Plymouth in the UK. He has more than 10 years of experience in the use of intraoperative ultrasound for HPB and general surgery. University Hospital Plymouth treats many patients with benign and malignant lesions in the liver, pancreas, and gallbladder.
Read More
Topics:
Intraoperative Ultrasound,
Laparoscopic Surgery,
Cholecystectomy,
HPB and General Surgery,
Minimally Invasive Surgery

-1.png?width=1200&height=630&name=MicrosoftTeams-image%20(21)-1.png)