Dr. David Carnovale is the medical director for fertility specialty care at Community Health Network in Indianapolis, Indiana, USA. He is board certified in obstetrics, gynecology, reproductive endocrinology, and infertility, with a specialization in reproductive endocrinology and infertility. One of the procedures he performs regularly is myomectomy, the preferred fibroid treatment for women who are trying to become pregnant.
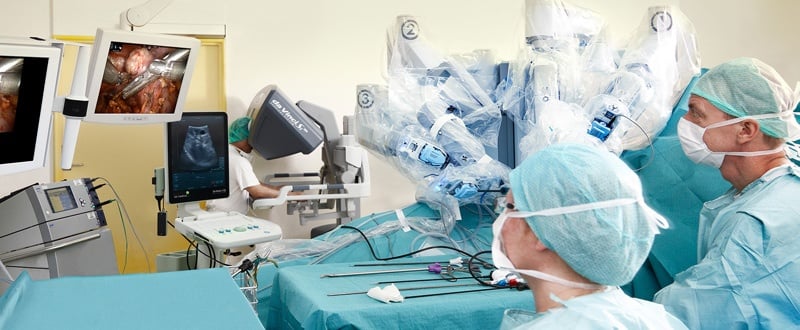
In 2010, Dr. Carnovale began performing robotic-assisted surgery and has since completed about 300 robotic cases. He uses this technology for myomectomy procedures and to treat endometriosis using laser. Dr. Carnovale advocates the use of intraoperative ultrasound for patients who are undergoing procedures for suspected fibroids, as he believes it provides advantages over other types of imaging that are available to his patients.
Why Dr. Carnovale Uses Intraoperative Ultrasound
“Ultrasound allows us to be less invasive during the patient’s surgical procedure,” he explained. “If we make a blind incision into a person’s uterus, thinking we know where the fibroid is, miss it and have to close that cut and make another incision, that’s a lot more invasive than having a very directed, real-time, ultrasound-guided incision that we know is going to be right on the mark. Ultrasound just brings so much more to the table in allowing us to be precise in where we make our cuts.”
While scanning the uterus during a myomectomy procedure, if a fibroid is embedded in the uterine wall itself and the contour of the uterus is distorted, it can become difficult to locate where to make the incision effectively. When this happens, surgeons may make an incision that they believe is over the fibroid only to find out that they missed the mark. With ultrasound, this is much less likely to happen.
One of the situations where Dr. Carnovale finds using intraoperative ultrasound especially critical is when a patient has a cavity distorting myoma and has endured multiple attempts to remove it hysteroscopically. “I’ve had patients come to me who had undergone two hysteroscopic procedures and still had a mass found at their next visit,” he said. “Flattened out myometrium containing the intramural portion of the myoma aggregates and balls up into a discreet mass once the portion that’s inside the cavity has been removed. By approaching from the pelvic side, we can use ultrasound to identify all of the mass, be more precise in removing the mass in question, and make sure the patient doesn’t have to undergo another surgery because something was missed.”
The use of ultrasound with myomectomies is especially critical for women who need to preserve their uterus because they may want to become pregnant. Ultrasound helps the surgeon ensure that no small fibroids are left behind to grow and require the patient to undergo further surgeries, risking more scar tissue. Additionally, the more times a uterus is operated on, the weaker it becomes and the less able a woman will be to carry a pregnancy safely. Removing all the fibroids at once improves the patient outcome.
Dr. Carnovale Explains The Setup He Uses for Intraoperative Ultrasound:
• The 12-5 MHz X12C4 transducer is sterile in the sterile field.
• The transducer is introduced through an accessory port.
• The location of the probe is manipulated with ProGrasp™ forceps (an instrument on the robotic platform).
• The ProGrasp is used overlying the X12C4 transducer probe instead of trying to approach it across the pelvis. This allows for easier manipulation and positioning of the ultrasound probe, assists with mapping the location of all the masses and helps plan all of the incisions that will be made.
• Once the location of the fibroid has been identified, the incision has been made, and the fibroid has been seen through the incision, the ultrasound is moved out of the field until the end of the procedure or if another fibroid needs to be located.
“At the end of the procedure, I always do a final ultrasound scan to make sure that no fibroids have been missed,” Dr. Carnovale explained. “This is very reassuring to the patient and the family because the last thing they want to hear is that you got ‘most’ of them out. They don’t want to know that they may have a fibroid remaining, no matter how small, because a year down the road when that fibroid grows they may need another surgery.”
Visit our surgery page to learn more about how our ultrasound systems can be used for intraopertive procedures. Click here to learn more about our new bk5000 surgical ultrasound system.